PLEASE NOTE: Our story contains many instances that may not reflect well on the medical teams that have actually saved our son’s life. Please understand that it is not my intention to bring negative attention to the wonderful people who work hard every day to save lives, but rather to create an awareness for all parents who have a child in the hospital.
Little Guy... Big Heart.
Zachary’s story.
Zachary’s story.
As parents of a healthy 2 year old, my husband and I had no reason to think that our second child would have any difficulties. We were excited to expand our family and everything seemed to be normal. We had our first ultrasound scheduled and had decided that we would like to know if we were going to have another boy or if we would need to start shopping for little girl things. Although we were unable to learn the gender of our baby, the ultrasound showed more concerning results. We were sent back to the exam room and my OB soon entered to tell us that it seemed as though our unborn child was missing a chamber of his heart. At that time, I was in no way, medically inclined. My husband had previous medical education so he understood more than I. The rest of my pregnancy included frequent doctor visits, fetal echos, and of course an amniocentesis, where we learned we were expecting another little boy. I quickly explored the internet to learn more about our unborn son and to find any info I could on Congenital Heart Defects or CHDs.
ZACH’S BIRTH
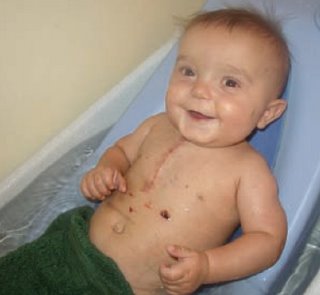
On February 12, 2003, Zachary Thomas Moore entered this world as expected, with only three chambers in his heart. He was born with Double Inlet Left Ventricle (DILV in the world of heart acronyms). To keep things simple, he had no right ventricle (*see below for a basic description of the heart and it’s blood flow). Since Zach did not have a right ventricle, both the right and left atrium were sending the blood to the only pumping chamber he had, the left ventricle. His oxygen poor and rich blood were mixing causing his oxygen levels to be extremely low and giving him a lovely blue/grey color to his skin. As his parents we saw a perfect little champion.
Many kids born with CHDs also have other defects and Zachary was no different. When I delivered him we realized he had a small “sack” at the end of the umbilical cord. This contained part of his small intestine. The medical world refers to this as an omphaocele. In addition, the intestines were malrotated and his small bowel was left “dangling” in his abdominal cavity, which can be fatal. We had no idea what we were in for... his abdominal defect would prove to be more of a challenge than his heart.
* After your body has circulated and used the oxygen in your blood it is returned to your heart through the right atrium, to the right ventricle. The right ventricle then pumps the blood to the lungs to re-oxyginate. The blood then moves from the lungs, through the left atrium, to the left ventricle which then circulates the oxygen rich blood back to the body.
SURGERY #1
Less than 24 hours after delivery we were being sent to the University of Minnesota (Riverside hospital) for further treatment. We were looking at a series of three heart surgeries that would happen over the course of 2-3 years, and what we thought was going to be only one abdominal surgery. The morning of Febraury 14th, Valentines Day, at two days old and weighing in at a whopping 5lbs 14ozs. our champion headed to the operating room for a Ladd procedure. This was the hardest thing we have ever had to do. To fix his omphalocele the surgeons had to “rearrange” his bowel. They found that there was a rupture and had to remove a small piece of his intestine. We were told that everything went well and less than 2% of kids that go through this procedure will have any additional abdominal troubles. GREAT! FIXED! Now let’s focus on his heart....
SURGERY #2
Shortly after his Ladd surgery we were transferred to the University of Minnesota (Campus hospital) to prepare for his first heart surgery. We were told that his heart function was going down hill and we needed to be on the surgery docket in case of emergency. Scheduled for the 18th of February, and told it couldn’t wait, we learned that our heart surgeon was out of town. Zachary had a Pulmonary Artery (PA) band placed, by another surgeon. The PA band was placed because there was too much blood flow to his lungs. This would tighten and restrict some of that flow. It is a simple (if you can call any heart surgery simple) procedure but they have to adjust the band just right, so it did take almost 4 hours. The next 24 hours were horrifying! We had fantastic nurses but learned quickly that as a parent of a “sick” child you have to pay attention, ask questions and make sure that you are on top of EVERYTHING!!!
That night we noticed that his medical chart had the wrong diagnosis, the diagram of his heart that the nurses used for reference was wrong, and remember... he had the wrong heart surgeon. Hours after surgery, Zachary’s sats began to drop and his team of nurses frantically worked to bring our boy back to us. He suffered a collapsed lung due to faulty equipment. That would come to be the first, of many times, I had seen my child “code”. Zachary recovered from the trauma well and every day I got to enter his room and see one less tube or one less IV. It made me cry. We were headed down the right road. After being transferred to an ICU closer to home we were finally discharged on February 28th.
HOME FOR THE FIRST TIME
The feeling of finally having our baby home and proceeding with a “normal” life, one without tubes and nurses and complications was absolutely amazing! We were not supposed to go back for his Glenn (the next heart surgery) until he was 6-9 months old. We got to put him in regular clothing instead of hospital gowns. He got to go outside and get some fresh air without bringing an IV tree with. The little things that parents take for granted every day became so important to us. We were keeping a close eye on him but trying not to treat him any differently than a well child. He had been loosing weight and having problems eating. No one would listen to me, I had told several doctors that he was having problems and there was something wrong with my baby. We saw his pediatrician and his cardiologist and were told that it was related to his abdominal troubles. After trying a few different medications, treating him for reflux, and being in and out of the hospital a few times we finally had the answer to his problems...
It was Mother’s Day, we were having our moms to our house to celebrate. In the process of getting food prepared and cleaning our home we put Zachary down for a nap. It was normal for our little champ to have crying fits, turn blue and pass out because of his heart and lack of oxygen. We were used to this. We heard him crying in his crib and then there was an awful, dead silence. Thankfully, my husband went to check on him and found the most heart wrenching site. Our boy was completely grey and not breathing. He had mucus out his mouth and nose and was completely limp. My husband brought him to me, laid him on the floor and began to administer CPR. I frantically called 911. By the time they arrived, which seemed like a lifetime, Rob had revived him and cleared his lungs. He had aspirated. They were on their way to the hospital again. Just as I had suspected, there was something wrong with our baby, and it wasn’t reflux.
This instance sent us back to the U of M for another 6 weeks and 3 more surgeries. We found that his original abdominal surgery (remember that 2%) had caused blockage. The reason that he had been projectile vomiting and having MANY messy diapers was because of his gut (on one occasion we changed more than 30 in one day). Even the surgeons were amazed.
SURGERY #3
His doctors had decided to do an “exploratory” procedure where they would go in and try to clean and reduce his adhesions that had formed to clear some blockage. It seemed to make things a little better. However it wasn’t enough to fix things completely. We were set for another abdominal surgery. In the meantime Zachary was running out of good veins. We had so many IVs, PIC lines, labs and had visited so many ERs that constantly poked and prodded they were worried about having the access that they needed.
His GI docs had decided that it was imperative that Zach have a central line placed. I was not a fan of this idea, something in me said that it was a bad idea. I had asked many questions and demanded that they explore every other option. In the end, the GI team had talked me into it.
SURGERY #4
They brought Zach to the OR for his central line placement. I know that this is a minor procedure but it is never easy to hand your child over for surgery, no matter how minor it is. As it turns out the complications from this surgery were the worst yet. I sat next to him in the ICU and watched his nurses “bag” him 6 times in one hour. The morphine was suppressing his respirations, relaxing him too much, he wasn’t breathing. From here on out we could no longer give him morphine and it was going to be tough to stay on top of his pain for future surgeries.
He now had a port in his chest that they told me would last through any troubles we had with him. That it would stay in for months and maybe even years, we wouldn’t have to poke him anymore. All of his medications could be administered through his line and all labs and blood tests could go through there too. What a relief!
SURGERY #5
Since the exploratory surgery hadn’t solved all of our problems we now had to send him in for a bowel resection. UNBELIEVABLE! Why didn’t people listen to me when I said there was something wrong? We might’ve been able to prevent this! When the surgeons got in the OR with him they found that almost 16cm of his bowel had dilated (ballooned) to almost 6cm in
diameter! No wonder his belly was distended. I knew that something wasn’t right. I was furious! And now after all of this we were going to bring Zach home with a port to maintain and clean. Or so we thought.
I got up one morning after Zachary had been doing really well, walked into his hospital room only to find that the GI docs were going to pull his line out. “The hell you are!” I believe those were my exact words. “I didn’t want it in the first place, you persuaded me, told me it was the best thing for him. He almost died in the ICU after that! You said we would keep it for his next heart surgery! And now you are going to take it out?” I didn’t know what to do! After my nurse calmed me down, she explained to me that the line HAD to be pulled. The GI team had never talked with his Cardio team. The catheter for the line was inserted into his heart in the exact same place they would need to access for his Glenn. In addition to that, if there were ever a clot the outcome could be deadly.
They had done it again. The people I had been trusting with our sons life had messed up again. He had a whole entire procedure that he never should’ve had, and almost died from it. Please keep in mind that I am very grateful that our son is alive today because of those same doctors. What is a parent to do? We didn’t want to “rock the boat” because the heart surgeon he was supposed to have originally came highly recommended and we still had 2 more surgeries coming. We had been paying attention, asking questions and even insisting on certain nurses and lab techs. We were doing all we could to make sure our son was given the best care. We never pursued anything. This had all been a huge learning experience and now we are working on ways to inform and educate other parents who may be in similar situations.
HOME AGAIN
This time everything was great! Zach was eating and playing and doing normal baby stuff.. I eventually forgot about all of the nightmares and the sleepless nights. I had just spent the better part of 5 months living at the Ronald McDonald house and 10-14 hours a day in a hospital room. His nurses had become my best friends. I had met so many families from all over the world that had kids that were suffering from similar (yet very different) illnesses. I had bonded with so many of those people that it was hard adjusting to being home. I was constantly thinking about the poor people that didn’t get to go home, the families that had been there longer than I, and were still there when I left. There were lots of kids in the hospital who were alone, whose parents for some reason or another were not there by their sides. I kept these kids and families in my prayers. But it was very difficult to stop thinking about all of the things we went through, and to change my schedule that I had known for so long. My responsibilities changed drastically, I had to get back into the lifestyle of being “normal”. I struggled, but with the help of my family, and to be able to bring Ethan (our 3 year old) his family back, made me smile.
SURGERY #6
We had a whole 4 months with him before we found ourselves back in the hospital for his Glenn procedure. With the exception of having a few minor complications from his heart catheter and troubles with pain control, we had a successful surgery. He had 2 superior vena cavas so it took them a little longer to complete the procedure. The biggest challenge was pain
control. Since Zachary was not allowed to take morphine we couldn’t keep him comfortable. We tried other meds but nothing seemed to work. The solution was pulling his chest tubes early. Not ideal, he needed to be monitored closely, but he came through it like a champ! After only about 10 days in the hospital Zachary had overcome yet another battle and we were set to go home.
SURGERY #7
Zachary is scheduled to have his Fontan on July 27th 2006. We are very nervous. Having been out of the hospital and healthy now since September of 2003 we are facing some new things with this surgery. Since Zach is so much bigger we will have to learn how to comfort him when he can actually tell us how much pain he is in. As an infant he wasn’t talking or running around, that will make his Fontan much harder to go through as a parent. We have been talking to him a little about it so I think he understands for the most part what is going to happen.
My family and I have kept in touch with families of CHD kids and have tried to help others understand what it is like to have a child in the hospital. I have spent time with friends and their kids in the ICU just to give them support and advice and to remind them that even though things seem hard and unfair at the time, look at my little Zach and all he went through... there is hope.
I am working on an informational web site for families of CHD babies and for anyone who would like to know more about caring for a sick child. I know how alone I felt the day of my first ultrasound when we were told about Zachary, and how comforting it was as I searched the internet to find others out there just like us. I hope to have the approval of our Cardiology
team and for them to pass our website on to other families expecting heart babies. Ideally, I would like for the site to become an outlet for Cardiologists across the nation to use as a a source of information for their patients.
We are very fortunate to have our little champion. He has taught everyone around us so much about life and it’s struggles. We have had friends and family members who look to our 3 year old for strength in their personal battles. He is an old soul here to help and inspire everyone he meets. He provides us with warmth and smiles everyday. He truely is a gift.
Feel free to contact me at any time with questions. This is a general overview of our time with Zach, many details have been omitted. I’d be glad to talk more about his story.
Thank you for this opportunity.
Rachael Moore
email: mooregraphic@gmail.com
www.caringbridge.org/visit/zacharymoore












No comments:
Post a Comment